Veterinary Advice: Vaccine Side Effects and Risks.
It is uncommon to see problems with the administration of vaccines to our pets, however issues with vaccination can occur and you should be aware of these when
planning to have a pet vaccinated. I must stress, however, that although the following problems and vaccine side effects can occur and can even be life threatening, vaccination safety is generally quite high and concerns and fears about the adverse effects of vaccines should not be used as grounds to avoid immunizing your cat or dog. The diseases that we are protecting them from (especially
canine parvovirus, canine distemper virus, canine adenovirus or hepatitis virus, feline panleukopenia - otherwise known as feline parvo or, incorrectly, feline distemper -
feline leukemia and feline immunodeficiency virus - otherwise known as FIV or feline AIDS)
can be far more disastrous than the real risk of a vaccine reaction.
The following article discusses these side effects of vaccination:
1) Sleepy, depressed, inappetent puppies and kittens immediately following vaccination.
2) Irritable, grumpy puppies and kittens that don't like being touched following vaccination.
3) A lump under the skin at the site of injection.
4) Nasal and/or ocular discharge and sneezing following intranasal vaccines.
5) Anaphylactic reactions.
6) Mild allergic reactions - puffy face and ears.
7) Vaccination failures - clinical signs of disease/infection despite vaccination.
8) Feline vaccine associated fibrosarcoma.
9) Lameness in kittens following the calicivirus vaccine.
10) Excessive bleeding at site of injection.
11) Concerns with pilonidal sinuses - caution in giving needles to Rhodesian Ridgebacks.
12) Immune diseases - e.g. Immune Mediated Hemolytic Anemia - following vaccination. Includes information on Serum Sickness.
13) Rabies vaccine reaction: neurological disease following administration of rabies vaccinations.
14) What do I do if my pet has a vaccine side effect?
WARNING - IN THE INTERESTS OF PROVIDING YOU WITH COMPLETE AND DETAILED INFORMATION, THIS SITE DOES CONTAIN MEDICAL AND SURGICAL IMAGES THAT MAY DISTURB SOME READERS.

Commonly Reported Side Effects of Vaccination
Sleepy, depressed, inappetent puppies and kittens:
When I worked at an Emergency Centre, one of the most common calls I used to receive
were from people whose kittens or puppies had just been vaccinated and which were
now listless and flat-seeming and wanting to sleep a lot. Some of them were reported to
feel 'hot to touch' and some of them were also off-food.
This general malaise after vaccination is a common sequelae to immunizing pups and, in particular, kittens (particularly
with the Feline Leukemia vaccine) and it occurs because the young body has just had a
highly immune-reactive, live virus injected into it (along with other reactive additives, called
adjuvants, which enhance the immune response) which the body is now busily
trying to fight off. As occurs with any infection that the body is fighting (think of yourself
with the flu), it is not uncommon for kittens and puppies to feel off-colour and lethargic, go off their food and even get a fever following immunisation. In my experience, the phenomenon tends to occur most when kittens and puppies have been given a large number
of vaccines to fight (e.g. kittens given the full course: feline herpes vaccination, feline calicivirus
vaccine, feline panleukopenia immunization, chlamydia immunization, feline leukemia vaccine, feline aids injection and, in some situations, a rabies vaccination as well).
When to worry:
In the first 24 hours after vaccination, I would not worry at seeing these post vaccine symptoms.
My suggestion would be to keep the kitten or puppy in a nice warm, quiet place, with plenty of water available (even gently syringing small amounts of water into the
mouth to get some liquid into them). Tempt them frequently with warmed, strong-smelling food
(e.g. fish or fishy canned food for cats, chicken for puppies) to get them to eat.
If they eat - great. They might be a bit off colour (not as playful or alert) for the next
couple of days as they fight the 'infection', but if they are eating and drinking well, then you can all probably ride it out without veterinary attention so long as the
animal continues to improve daily. If the young animal will not take food or water, then this is of greater concern. Young kittens and puppies are only small and can dehydrate
quickly. My advice is that if the pup or kitten has not picked up and started drinking and eating by 36 hours (at the latest 48 hours), you should seek veterinary advice.
NOTE - Live attenuated vaccines containing Chlamydia can cause signs of fever, lethargy and stiffness for up to three weeks in kittens, following vaccination with these products. It is usually self limiting but pain relief and anti-inflammatories may help to make the kitten more comfortable while the problem resolves itself.
Irritable, grumpy puppies and kittens that dislike being touched:
It is not uncommon for vaccine sites to hurt after vaccination. After all, the
injection site of a vaccine is a site where an aggressive immune inflammatory response is taking place and, consequently, the region can be swollen, red and
painful. Petting a kitten on the neck or head after vaccination can often elicit a flinch, accompanied by a growl or cry. Owners can be bitten or scratched
if they touch the sore vaccination spot. In addition to the pain of the site, these
kitties and puppies are often a bit feverish and off-colour: this does not improve
their mood!
Remember also, that some of the vaccines are given in the hind legs (right hind leg for
rabies vaccination and left hind leg for feline leukemia vaccination). Kittens and
puppies injected in a leg will often be painful to touch in these places and may also
limp.
When to worry:
In the first 3-5 days, I would not be concerned. If, however, a large lump forms
at the site and seems to be getting larger (e.g. an abscess) OR the animal becomes unwell, off food, depressed etc. outside of that initial 24-48 hours immediately after the vaccination, I would see a vet immediately. Injection site infections can occur.
A firm, non-painful lump under the skin at the site of injection:
It is not uncommon, particularly with killed vaccines containing reactive adjuvants (immune system stimulatory additives), to get a lump at the site of vaccination. Generally this lump is under the skin
and can be quite mobile. Often somewhere around the size of a pea, right up to the size of a large marble,
these vaccine-site-reaction lumps are comprised of a mixture of inflammatory cells
(the immune system cells that attacked the injected vaccine) and scar tissue. They may stay the same size for years or can, over time (generally 2-6 weeks), reduce in size. Some will even disappear. In some breeds (e.g. poodle, bichon), these reactions can be associated with dark skin pigmentation and loss of hair at the site of the vaccine. Many veterinarians
will vaccinate show dogs in discrete areas (inside the groin, under the point of the shoulder) to
avoid vaccine-associated lumps or hairloss being picked up by judges at shows.
When to worry:
If the lump grows very large within the first month of vaccination (particularly
if the lump is red and painful or the animal is off colour), I would advise veterinary attention. Not all vaccine lumps are typical vaccines site reactions: abscesses can occur if the vaccine was contaminated with bacteria or if bacteria from the skin was inadvertently pushed under the skin by the vaccine needle. Abscesses need veterinary attention.
Also, if the lump stays one size for ages and then, inexplicably, starts growing in size, I would definitely advise checking this. It is possible for cancers (e.g.
feline vaccine associated sarcoma) to form at sites of inflammation, including
vaccination inflammation. For this reason, you should make a habit of regularly palpating
and noting the size of any lump present on a pet.
Nasal and/or ocular discharge and sneezing:
Live intranasal vaccines including the kennel cough vaccines (parainfluenza virus, Bordetella +/- canine adenovirus) and intranasal cat flu vaccines (feline
herpes virus - FHV - and feline calicivirus - FCV) can induce mild signs of the disease that they are designed to prevent, with a watery ocular and nasal discharge and sneezing (occasionally coughing) being the most common signs. These signs tend to develop 3-4 days following intranasal vaccination.
When to worry:
 Generally, these symptoms are self limiting and disappear within days. If the nasal discharge thickens and develops colour, changing from a clear, watery
discharge to a thicker yellow or green discharge, a visit to the vet is warranted. Green
and yellow discharges can be indicative of bacterial infection and antibiotic medication may be needed.
Generally, these symptoms are self limiting and disappear within days. If the nasal discharge thickens and develops colour, changing from a clear, watery
discharge to a thicker yellow or green discharge, a visit to the vet is warranted. Green
and yellow discharges can be indicative of bacterial infection and antibiotic medication may be needed.
Note that it is possible for cats and dogs showing mild vaccine-induced respiratory symptoms to pass these vaccine viruses on to other cats/dogs in the household, thereby inducing similar mild upper respiratory tract symptoms.
Note that, in populations of cats and dogs with genetic immunodeficiencies (e.g. some purebred animal breeds), the use of intranasal vaccines may need to be avoided becaue of a greater risk of severe upper respiratory signs being induced by nasal vaccinations.

Less common vaccine Side Effects:
Anaphylactic reaction:
Anaphylaxis is a severe, life-threatening allergic reaction that occurs against one or more components of the vaccine. When exposed to the foreign reactants (called antigens and adjuvants) contained in the vaccine, the mast cells of the immune system activate, releasing massive amounts of histamine into the system.
In dogs, this results in acute vomiting and diarrhoea (sometimes containing blood), severe, acute shock, collapse, pale grey/white gums, a rapid heart-rate and low blood pressure. Animals can even 'drop dead' (severe allergic reactions towards vaccines are responsible for many of the vaccine deaths encountered by vets). Swelling of the face and throat can occur, making it very difficult for the
dog to breathe. Wheals or 'hives' (raised red patches) can occur over the skin.
In cats, vomiting, diarrhea, sudden collapse and itchiness of the face (+/- swelling of the ears) can occur as they do in dogs. Cats can sometimes get a severe, life-threatening reaction within their lungs, resulting in fluid (and even blood) pooling within their airways. This lung condition may progress despite treatment and result in death of the cat.
Any vaccine has the potential to cause a reaction, however, it should be noted that the killed vaccines (e.g. killed rabies vaccine, FeLV vaccines) are possibly more likely to induce an allergic vaccine reaction than the live vaccines. This is because the killed vaccines often contain large amounts of viral material (they don't replicate in the body so more has to be injected initially) as well as adjuvants (additives that stimulate a better immune reaction) which are both very immunoreactive. Killed bacterial vaccines (termed bacterins) such as the Bordetella injectable vaccines, coronavirus vaccines and leptospira vaccines are also highly reactive and likely to cause allergic reactions.
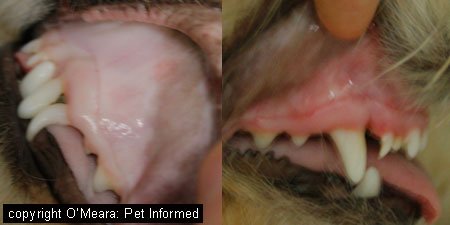
Image of gum colour before and after anaphylaxis treated with antihistamine.
When to worry:
Anaphylaxis is an emergency and must be seen immediately by a vet. Often the reaction occurs in the vet clinic (sometimes within seconds of vaccination) or soon after the animal has left the clinic, although it can take up to 24 hours to manifest (so you should keep a close eye on the animal at home). The vet will usually rush the dog straight out to a treatment room, where it will receive oxygen, IV fluids, anti-histamines, adrenaline, anti-inflammatories and sometimes other drugs to aid in the treating of low blood pressure.
Generally, if a dog or cat survives an anaphylactic reaction, it should be fine. Very old animals that suffer shock reactions may be at risk of developing acute renal failure
or other systemic signs due to the drop in blood pressure that occurs and they should
be monitored for this over the next 24-48 hours. Pregnant bitches or queens may abort.
The issue is then, do we vaccinate the animal again?
Generally, vets will try to keep the annual vaccinations going in younger animals (under 6-8 years)
because of the risk of infection from the viruses if they are unvaccinated and because
of the fact that under vaccinated animals (pets that have not received their booster
vaccinations) will not be accepted by kennels and catteries.
Generally what happens is that:
1) the vet will premedicate the animal with an antihistamine 5-15 minutes prior to vaccination (to try to reduce the risk of severe reaction). He will rarely use an
anti inflammatory such as a corticosteroid, because these products suppress the immune system response, possibly making the vaccine less effective.
2) the veterinarian will vaccinate the animal using either a different
brand of vaccine (e.g. change from a CSL vaccine to a Fort Dodge vaccine); a different
form of vaccine (e.g. live instead of killed); a different vaccine schedule (e.g. several vaccines over several days to reduce the amount of reactive material being given all at once); a different route of administration of vaccine (e.g. go from an injectable to an intranasal, which is not taken up as rapidly into the body) or some combination of all of these. Use of the new three-yearly vaccines is indicated here because, even if a mild reaction
occurs, the dose will not have to be repeated for three years.
3) the vet will then monitor the animal in the clinic for any reaction. You may be
required to leave your pet at the vet for a period of time to be watched.
 If the animal is older (over 8 years), the vet may elect to discontinue the yearly vaccination of the animal (especially if it does not attend kennels). The older animal is likely to have built up good immunity towards the main life-threatening diseases (distemper, parvo, adenovirus) and will hopefully be fine. The dog will still be
at risk of kennel cough, but an intranasal form of the kennel cough vaccine could be tried here
instead of the injectable.
If the animal is older (over 8 years), the vet may elect to discontinue the yearly vaccination of the animal (especially if it does not attend kennels). The older animal is likely to have built up good immunity towards the main life-threatening diseases (distemper, parvo, adenovirus) and will hopefully be fine. The dog will still be
at risk of kennel cough, but an intranasal form of the kennel cough vaccine could be tried here
instead of the injectable.
It is possible for some laboratories to measure the level of specific antibodies (proteins in the immune system that recognise viruses in order to trigger immune system defense systems) toward certain infectious organisms, contained in your dog or cat's blood. If antibody levels towards certain organisms are high enough, the animal is considered adequately protected and should not need a vaccine at this time. Antibody measurements can be done on older dogs or younger dogs to assess which vaccines are required. If easily available, these tests should be performed on all animals that have had a vaccination reaction, prior to their next vaccine, so that only the necessary vaccines are given.
How do you know which vaccine caused the reaction?
Since all of the vaccines tend to be given at the one time, it can often be impossible to tell which vaccine was the culprit so you have to careful giving any
of them. At the next vaccination, you could consider having the vet give each component a few days apart (where individual virus vaccine products are available) to try to tell which, if any, is the problem. You might potentially
find that it is something else (e.g. the heartworm needle) and not the vaccine that
caused the problem.
Alternatively, your vet can do an intradermal skin test (0.1ml of each vaccine is administered in the skin) to see which vaccine induces an skin reaction response (a large wheal at the site of injection) as one way of trying to identify the culprit vaccine.
Note that, if the animal has reacted after being given a rabies vaccine, regardless of age you
may still be required to vaccinate the dog yearly. This depends on individual state and country laws.
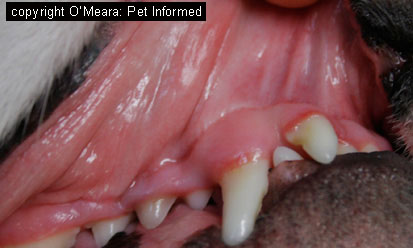
Mild reactions - puffy face and ears:
Sometimes after a vaccination, the animal will not develop a severe anaphylactic
reaction, but will show signs of a mild allergic reaction including a puffy face, swollen eyelids, swollen lips and ears (cats especially get puffy ears), itchiness (they'll rub their face and scratch
their bodies) and sometimes wheals/hives all over the body. Generally, these animals
will not progress to anything nasty, but they will be very uncomfortable - red, hot and itchy. As long as their gum colour remains normal (nice and pink - see image), they show no signs of trouble breathing or wheezing and they are otherwise bright and alert, you may not need to see a vet - the signs will usually abate within a day, sometimes within hours. If the dog is very uncomfortable and distressed from the itching, however, you can see a vet and s/he will check your pet over and give
them a dose of an antihistamine. This will speed the onset of normality.
Can I revaccinate my pet after a mild allergic reaction?
In the case of mild reactions and re-vaccinating your pet, one of three things could happen:
A) the animal may have the exact same, mild reaction next time,
B) the animal may have no reaction OR
C) the animal could progress and have a severe anaphylactic reaction and collapse.
I would tend to err on the side of caution and assume that the third option is the likely one. As a result, I would tend to treat subsequent vaccinations with as much caution as I would if the animal's first reaction had been severe anaphylactic.
I would take the same precautions for re vaccination (antihistamine premed, try a different
vaccine, monitor the animal afterwards etc.)
Vaccination failures - clinical signs of disease despite vaccination:
We will soon link to a whole page dedicated to vaccine failure, but the following is a good, general summary.
Occasionally, vaccines administered by veterinarians will not have the desired prophylactic
(preventative) effect and the animal will develop signs of the vaccinated-for disease/s. This can
occur for two main reasons:
1) The disease seen is being caused by the vaccine itself:
With some live vaccinations (especially the intra nasal vaccines) it is not uncommon for the
animal to develop mild signs of disease: nasal discharge, watery eyes, sneezing. These should, however, be mild and self limiting.
If an animal develops major signs of infection immediately following vaccination with a live attenuated virus vaccine (e.g. a dog develops full-blown parvovirus) then my suspicion would be that the animal had either already been exposed to the wild-type virus
around the time of vaccination (i.e. before vaccine immunity was achieved) OR that
there was some kind of problem with the animal's own immune system making it unable to fight off the 'mild' vaccine virus strains. It is for this reason that one of the major vaccine contraindications is the use of live vaccines in immune suppressed animals
including pregnant bitches/fetuses; very sick animals; animals on chemotherapy and animals on immune suppressant medicines. Infection should not be possible from killed virus vaccines.
2) The disease seen is being caused by a wild-type virus - i.e. a true vaccination failure.
Vaccination failure can occur for many reasons, including:
- the presence of long-lived maternal antibody in the pups, preventing the puppy immune system from being exposed to the vaccine
- a new strain of wild-type virus that is not protected against by the vaccine-induced immunity
- exposing pups to the public (and viruses) before they have finished the full vaccination course and gained immunity
- incorrect vaccination procedures - freezing vaccines, leaving vaccines in the sun, using out-of-date vaccines, not following recommended vaccine protocols, vaccinating febrile or cold animals (e.g. animals under anaesthesia)
- incorrect vaccine administration - not getting intranasal spray vaccines into the nose etc.
- exposure to very large levels of wild-type virus (massive virus loads can overwhelm the immune system)

Rare vaccine side effects:
Feline Vaccine associated fibrosarcoma:
Fibrosarcomas are nasty cancers comprised of mutated, uncontrollably-dividing connective tissue cells that can appear anywhere on the body, including sites of prior vaccination. Occurring at a miniscule rate of 1/1000 to 1/10000 vaccinated cats, anywhere from 2 months to 3-4 years after vaccination (the canine rabies vaccine and feline leukemia vaccine are
said to be the main culprits), vaccine associated sarcomas are extremely aggressive, locally invasive tumours that send long 'fingers' of cancer cells out into surrounding tissues.
Left untreated, these tumours can invade deeply into the body and wind up killing the cat.
When to worry:
Make a regular habit of palpating the vaccine sites of your cat - don't forget to
feel the hind legs as this is where the rabies and feline leukemia vaccines are
commonly given. If you feel a lump at an injection site that seems to be enlarging (especially
if it develops more than a month after vaccination) or which is greater than 2cm, get it seen by your vet. A good biopsy will diagnose a sarcoma and early and aggressive surgical treatment is often curative.
How do you treat feline vaccination associated sarcoma?
Because connective tissue tumours are generally poorly responsive to chemotherapy (cancer medicines), the best means of treatment of sarcomas is usually excision (cutting it out) sometimes followed up with radiation. Because these tumours tend to be very locally invasive, a radical excision (surgery to cut out the mass) with very wide margins is
required to try to get rid of the 'fingers' of cancer cells. If any cancer is left behind, which is likely with large advanced tumours (hence the importance of getting it seen to early), the mass will soon grow back. If the tumour is located on a hind leg, amputation of the leg is often curative - it is for this reason that the rabies and
leukemia vaccines (the main cancer culprits) are administered in the hind leg. In some cases where complete excision has been impossible, follow-up treatment with radiation over 3-4 weeks may allow a cat to live for several years.
Prevention of vaccine associated fibrosarcomas:
There is no way to completely prevent these from occurring,
short of not vaccinating the cat at all. Note, however, that not
giving the vaccine is an option with certain immunisations. Obviously, if you do not live in a rabies-endemic region you probably don't need to vaccinate against rabies (check your local laws though). The same with feline leukemia: a cat that exists 100% indoors with no other cats is very unlikely to ever get feline leukemia virus. With the other core vaccines, although you still need to give them, you can reduce the frequency of vaccination by testing the cat's protective antibody levels to see if a cat needs a vaccine.
If you do need to vaccinate, the risk can be reduced by not giving multiple vaccines in just one site. The more immune stimulation that occurs in one site, the greater the risk of potentially cancerous cell transformation.
The use of live vaccines rather than killed vaccines may be preferable too as the killed vaccines often contain a lot of additives (called adjuvants)which induce an aggressive inflammatory response at the site of injection, possibly leading to neoplasia (cancer). This is of particular concern with the aluminium-containing adjuvants: they should be avoided. There are now non-adjuvant-containing FeLV (feline leukemia) vaccines and rabies vaccines, which may be a lot safer.
You should palpate your cat's injection sites regularly to detect early lump formation.
Vets should give feline leukemia and feline rabies vaccinations in the hind legs (right rabies, left leukemia) so that a leg can be removed should a tumour develop. Also, vaccines should ideally not be given in the scruff of cats (between the shoulderblades) because tumours in this area are tricky to cut out and vaccines tend to pool here, leading to a prolonged, focal reaction against the vaccine in this region. Vaccines should also be given under the skin, not in the muscle, because skin lumps are easier to detect. Vets should also keep a record of the injection sites used (which vaccines are used and where) and keep to this pattern for all subsquent boosters so that recognition of vaccine sites will be much easier.
Intranasal vaccines, where available, should be used in place of injectable vaccines as they are not as implicated in the formation of vaccine sarcomas.
Note - fibrosarcomas are not the only type of cancer that can occur at a vaccine site. Tumours comprising bone cells (osteosarcomas), muscle cells (rhabdomyosarcomas), cartilage cells (chondrosarcomas) and many other cell types have been found.
Lameness in kittens after the calicivirus (FCV) vaccination:
Feline calicivirus is well known as a cause of 'cat flu' symptoms - sneezing, eye discharges, nasal discharges and mouth and tongue ulcers. Less commonly, the virus also affects
the bones and joints of the kitten, causing joint swelling, joint pain, muscle soreness
and fever. They often limp and they resent having the limbs handled or palpated. The
symptoms generally resolve in 2-4 days without any medication. The reason that this
information has been placed in the vaccination side effects section is that, sometimes, the live feline calicivirus vaccine can induce the same self-limiting 'limping kitten' signs generally within 1-3 weeks after vaccination.
When to worry:
Any kitten that is feverish, lethargic, inappetent and lame in multiple limbs should be examined by a vet. If it is due to the calicivirus vaccine, good news: it will generally resolve within 4 days without any need for medicine (though fluids, pain-relief and antibiotics can be provided to support them), but I would still advise getting the kitten checked
over because there are other nasty illnesses (e.g. immune polyarthritis) that can
present with similar signs.
Excessive bleeding at site of needle or vaccination:
It is not common, but I have encountered cases where a dog or cat is given a needle
(any type of needle, including a vaccine) and then keeps on bleeding from the site of injection. A huge bruise or blood-filled lump (called a hematoma) may even develop on the skin at the injection site.
These cases are not normal and are not an effect of the vaccination needle or administration of vaccines per se. Generally
what happens is that the animal has an underlying bleeding disorder (the animal
can not clot its blood) that was unknown before the vet stuck the needle in. Common causes include: rodenticide poisoning (the animal has eaten rat or rabbit poison); human
anti coagulant consumption (the animal has eaten the owner's warfarin), blood platelet
deficiencies (e.g. immune system attack on the platelets) or congenital bleeding
disorders (hemophilia, von willebrand's disease).
When to worry:
Any injection site or cut that does not stop bleeding or that bruises excessively is cause for concern. Animals with normal blood clotting abilities do not do this!
Your vet needs to check for an underlying bleeding disorder.

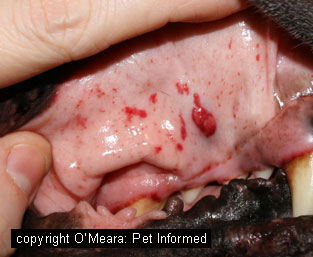
Image 1: rodenticide poison. Image 2: bruising on the gums caused by platelet deficiency
Rhodesian Ridge back or Rhodesian crossbreds - issue with injecting into pilonidal sinuses:
At university, it was drummed into us to never inject along the ridge of a
ridge back - or any breed with the ridge along its back, in case the dog had a pilonidal sinus. A pilonidal sinus is a birth defect present in the ridge back and some other breeds whereby the skin and spinal canal of the embryo do not completely
separate from each other in utero, resulting in a narrow passage lined with skin cells
remaining between the skin and the spinal canal. The skin cells in the passage can make
hair or skin flakes (dander) which can extrude out through a hole in the skin surface.
In most animals, this is not a clinical problem: owners learn to express and clean the area that the debris comes out of, but in some animals the sinus is a major issue, resulting in abscessation (infection which can impinge on the spine) and neurological signs.
The issue with vaccination or any needle for that matter comes if someone accidentally
injects substances into the sinus. Since the pilonidal sinus communicates with
the spinal canal, injections into the 'ridge' can potentially result in injection fluid leeching down into the spine. This has the potential to cause neurological damage, infection or even death (depending on the stuff injected).
How to avoid it:
Don't inject ridge back or ridge back cross breds anywhere along the dorsal body, particularly within the ridge and even more particularly within the 'whorls' of
the ridge (as these whorls are often where the sinus exits the body).
Immune mediated hemolytic anemia (and other immune diseases) following vaccination:
Immune mediated hemolytic anemia is a severe, life-threatening disease whereby the
immune system targets and destroys the red blood cells of the body, resulting in anemia, jaundice (yellow gums), pale gums, weakness and sometimes fever. Animals can be so severely anemic that they need blood transfusions to stay alive and some may
die as a result of anemia and lack of oxygen to tissues or as a result of blood clots
entering the lungs, brain or kidneys (ruptured red blood cell membranes float around causing
clots to form). These animals are sometimes very sick and in need of special veterinary care and immune-suppressive medications in order to recover. Some will
not recover despite what we do.
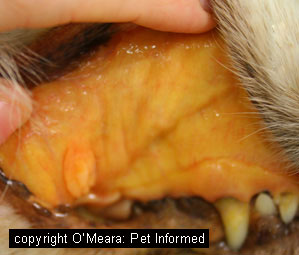
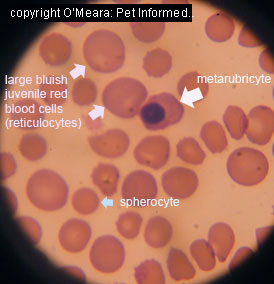
Image 1: yellow, pale gums typical of severe IMHA, Image 2: blood smear from dog with IMHA,
Shortly, Pet Informed will be bringing you a whole series on immune mediated hemolytic
anemia and its treatment, as it is one of the more common serious disease issues encountered in the dog or cat. The reason I have included mention of it here is that
there are many reasons why the immune system gets triggered to attack the body's red blood cells (or other organ systems - e.g. joint, kidney) and one of these
causative factors is thought to be vaccination. For some reason, vaccines can sensitise the immune system in such a way that the immune system gets confused and starts attacking cells of the body.
When to worry:
Any dog with pale or yellow gums must be seen by a vet. These signs will often be accompanied by variable signs of lethargy (tiredness), low exercise tolerance, collapse, dark coloured urine (the urine is often deep yellow, red - the colour of port wine - or brown), heavy or rapid breathing and sometimes inappetence and fever.
Aside from attack on the red blood cells, vaccination can potentially induce the immune system to mistakenly attack other cells in the body, resulting in other immune-mediated diseases besides hemolytic anemia. Example 1: the immune system could be triggered to attack the blood platelets, resulting in a reduced ability to clot the blood and widespread bruising and bleeding within the body. Example 2: the immune system can attack the nerves supplying muscles of the limbs and head (this is termed polyradiculoneuritis or Coonhound paralysis) resulting in flaccid paralysis (a floppy dog) and wasting of the muscles that can progress to affect the dog's ability to breathe and swallow. The affected dog may require months of supportive care (including ventilation and tube-feeding) to recover. See the next section on rabies reactions for more information on polyradiculoneuritis - although it can potentially occur with any vaccine, the condition is particularly associated with the rabies vaccines.
Vaccine-induced Serum Sickness - a rare form of immune-mediated disease:
Sometimes, instead of the immune system being 'tricked' into attacking the body's own cells, it is possible for vaccines to induce 'immune disease' by virtue of where antibody/vaccine-virus-antigen complexes decide to deposit themselves.
When a vaccine antigen (the virus protein and/or vaccine additive that the immune system is meant to recognise and attack) is injected into the body, it gets recognised by immune system antibodies. These antibodies bind to the antigen (this binding of antibodies to antigen is called an immune complex) and then, through a series of cell reactions, call other immune system cells over to attack the antigen. This is how an antigen (e.g. an infectious virus) gets destroyed by the body so that it can't cause disease: it is a natural process and vital to the survival of an animal.
Where it all goes wrong: sometimes immune complexes float through the body and get deposited in narrow blood vessels. These narrow vessels are particularly numerous in areas of the body such as the joints, brain, kidney and retina (back of the eye). When the antibodies contained in the immune complexes call the inflammatory cells over to 'kill' the antigens, this immune attack takes place inside these fragile, narrow vessels, resulting in injury of these vessels and their associated organs. Termed serum sickness, this phenomenon can result in painful inflammation and swelling of the joints (called polyarthritis), inflammation and damage to the eye (called uveitis), inflammation and injury of the kidneys (especially the kidney blood-filtering regions called glomeruli) and potentially damage to numerous other organs. Death is possible.
Note - Some Akita lines show signs of multiple-organ immune-mediated disease (including polyarthritis, fever, non-regenerative anemia, renal damage and liver injury) generally within 1 month of vaccination. These dogs often need lots of immune-suppressant drugs to treat the condition and many will die from progressive renal failure.
Rabies Vaccine Reaction: Neurological disease following administration of rabies vaccinations:
It is possible for a dog or cat to develop vaccine-induced form of rabies 10-21 days after receiving a live virus rabies vaccine.
In dogs, one of two things may happen:
The dog could develop a flaccid paralysis of the limbs (a floppy dog) which mimics other diseases like tick paralysis, botulism, snakebite and organophosphate toxicity in appearance, but which is closest
in nature to the disease Coonhound paralysis: an immune attack on the nerves supplying
muscles of the body, such that the animal is paralysed. (Note the similarity between
this and the previous section - immune system attack on red blood cells caused by vaccination - the immune system can be overly sensitive to vaccines). These rabies-vaccinated animals, if supported well for up to 3 months (e.g. nutritional support, possible ventilatory support) may get better.
Rabies vaccinated dogs can also get a severe infection of the brain and spinal cord (called encephalomyelitis)
which mimics the rabies disease itself. Any part of the nervous system can be affected and so neurological signs can be very variable. This condition will progress and there is no cure.
In cats (and also some dogs), what is encountered is a flaccid paralysis starting at the leg in which the vaccine was given. This progresses to the other hind leg (cat ends up dragging the hind legs)
before eventually involving the forelegs (cats show rigid stiffness of the limbs) as well as the brain (cat shows dementia). There
is not cure for this progression and the cat will either die or need to be euthanased.
How do we prevent this?
The vaccine-associated rabies does not seem to occur with the killed / inactivated vaccine,
only the live vaccines (live attenuated vaccine), so prevention is possible by using killed vaccines.

What Do I Do If My Animal Has a Reaction?
If an animal has a reaction from a vaccine, it is a good idea to always notify your
vet of the problem, even if it is just one of the mild self-limiting reactions
noted in the above sections. This way, your vet can report it on your pet's clinic notes so that future vets are aware of the possibility of there being a problem.
With issues like severe anaphylactic reactions, clinic notes that make other vets and nurses aware of the risks of vaccination exposure could well save your pet.
Any time that you take your pet to the vet in the future (especially if the veterinarian
that you see is not your normal vet) you should remind them of the dangers of vaccinating
your pet.
The vet should also notify the maker of the vaccine (vaccine manufacturer) about the
reaction so that the company has feedback about their vaccines. Drug companies are generally
very responsible and they use this kind of information to troubleshoot and improve upon their vaccines.
The vet will notify the company of the batch-number of the vaccine (a label that
appears on your vaccine certificate - see image). If a company gets a lot of complaints
about a particular batch, they might even recall it, saving other pets from being given a potentially dangerous vaccine.



Summary of Vaccination Risks and dangers - Take Home Messages:
Vaccination reactions and illnesses can occur but, as they are uncommon, the fear of a
reaction (unless it actually occurs) should not be reason enough to avoid vaccinating
dogs and cats. The diseases that we are protecting animals from can often be far worse than the miniscule chance that a vaccine reaction or side effect will occur: the benefits of vaccinations do
outweigh the vaccination risks.
It is common for puppies and kittens to be a bit sleepy, grumpy and lethargic the day
or two after vaccination.
Make a habit of palpating vaccination sites regularly for any lumps that form and, if these lumps seem to be growing, seek veterinary attention.
Rabies and feline leukemia vaccines are the ones most implicated in vaccine associated sarcomas
and should be given at separate sites in the hind legs.
Vaccines sometimes stimulate the immune system excessively, causing the immune system
to attack cells of the body. Disease situations such as immune mediated hemolytic anaemia (IMHA), immune mediated thrombocytopenia (IMT or ITP), polyradiculoneuritis (Coonhound
paralysis or vaccine-associated-rabies), polyarthritis (joint inflammation) and many others can result.
Report any vaccine reactions or side effects to your vet.

To go from Vaccine Side Effects page to Home Page, click here.

References and Suggested Readings:
1) Encephalitis, Myelitis, and Meningitis. In Nelson RW, Couto CG, editors: Small Animal Internal Medicine, Sydney, 1998, Mosby Inc.
2)Fenner WR, Diseases of the Brain. In Ettinger SJ, Feldman EC, editors: Textbook of Veterinary
Internal Medicine, Sydney, 2000, WB Saunders Company.
3) Wolf AM, Other Feline Viral Diseases. In Ettinger SJ, Feldman EC, editors: Textbook of Veterinary
Internal Medicine, Sydney, 2000, WB Saunders Company.
4) Kraegel SA, Vaccine-Induced Sarcoma in Cats. In Ettinger SJ, Feldman EC, editors: Textbook of Veterinary
Internal Medicine, Sydney, 2000, WB Saunders Company.
5) White RAS, Surgical Treatment of Specific Skin Disorders. In Slatter D, editor: Textbook of Small Animal Surgery, Philadelphia, 2003, Saunders.
6) Greene CE, Schultz RD, Immunoprophylaxis. In Greene CE, editor: Infectious Diseases of the Dog and Cat. St. Louis, 2006, Saunders Elsevier.
Article copyright Pet Informed (TM): February 2008.
All rights reserved, protected under Australian copyright. No images or graphics on this Pet Informed website may be used without written permission of their owner, Dr. O'Meara.
Protech, Duramune, Fort Dodge and Fel-O-Vax are registered trademarks of Wyeth and its affiliates.
Nobivac and Companion are registered trademarks of Intervet.
Adrenaline Injection BP is a product of AstraZeneca.
Niramine is a registered trademark of Jurox.
Tomcat and Blox are registered trademarks of Bell Laboratories Inc.
Any dose rates mentioned on these pages should be confirmed by a vet. Dosing rates for common
drugs are being changed and updated all the time (e.g. as new research comes in and as drug
formulations change) and information here may not remain current for long. What's more, although we try very hard to maintain the accuracy of our information, typos and oversights do occur. Please check with your vet before dosing any pet any medication or drug.
 Generally, these symptoms are self limiting and disappear within days. If the nasal discharge thickens and develops colour, changing from a clear, watery
discharge to a thicker yellow or green discharge, a visit to the vet is warranted. Green
and yellow discharges can be indicative of bacterial infection and antibiotic medication may be needed.
Generally, these symptoms are self limiting and disappear within days. If the nasal discharge thickens and develops colour, changing from a clear, watery
discharge to a thicker yellow or green discharge, a visit to the vet is warranted. Green
and yellow discharges can be indicative of bacterial infection and antibiotic medication may be needed. 


 If the animal is older (over 8 years), the vet may elect to discontinue the yearly vaccination of the animal (especially if it does not attend kennels). The older animal is likely to have built up good immunity towards the main life-threatening diseases (distemper, parvo, adenovirus) and will hopefully be fine. The dog will still be
at risk of kennel cough, but an intranasal form of the kennel cough vaccine could be tried here
instead of the injectable.
If the animal is older (over 8 years), the vet may elect to discontinue the yearly vaccination of the animal (especially if it does not attend kennels). The older animal is likely to have built up good immunity towards the main life-threatening diseases (distemper, parvo, adenovirus) and will hopefully be fine. The dog will still be
at risk of kennel cough, but an intranasal form of the kennel cough vaccine could be tried here
instead of the injectable.





